Thousands of women at an increased risk of ovarian cancer are, for the first time, being offered the chance on the NHS to delay surgery, allowing them the potential to have a baby and avoid early surgical menopause.
 4m
4m
Thousands of women at an increased risk of ovarian cancer are, for the first time, being offered the chance on the NHS to delay surgery, allowing them the potential to have a baby and avoid early surgical menopause.
Instead of an operation to remove their ovaries, they are being tested every four months to monitor their risk and catch the disease early.
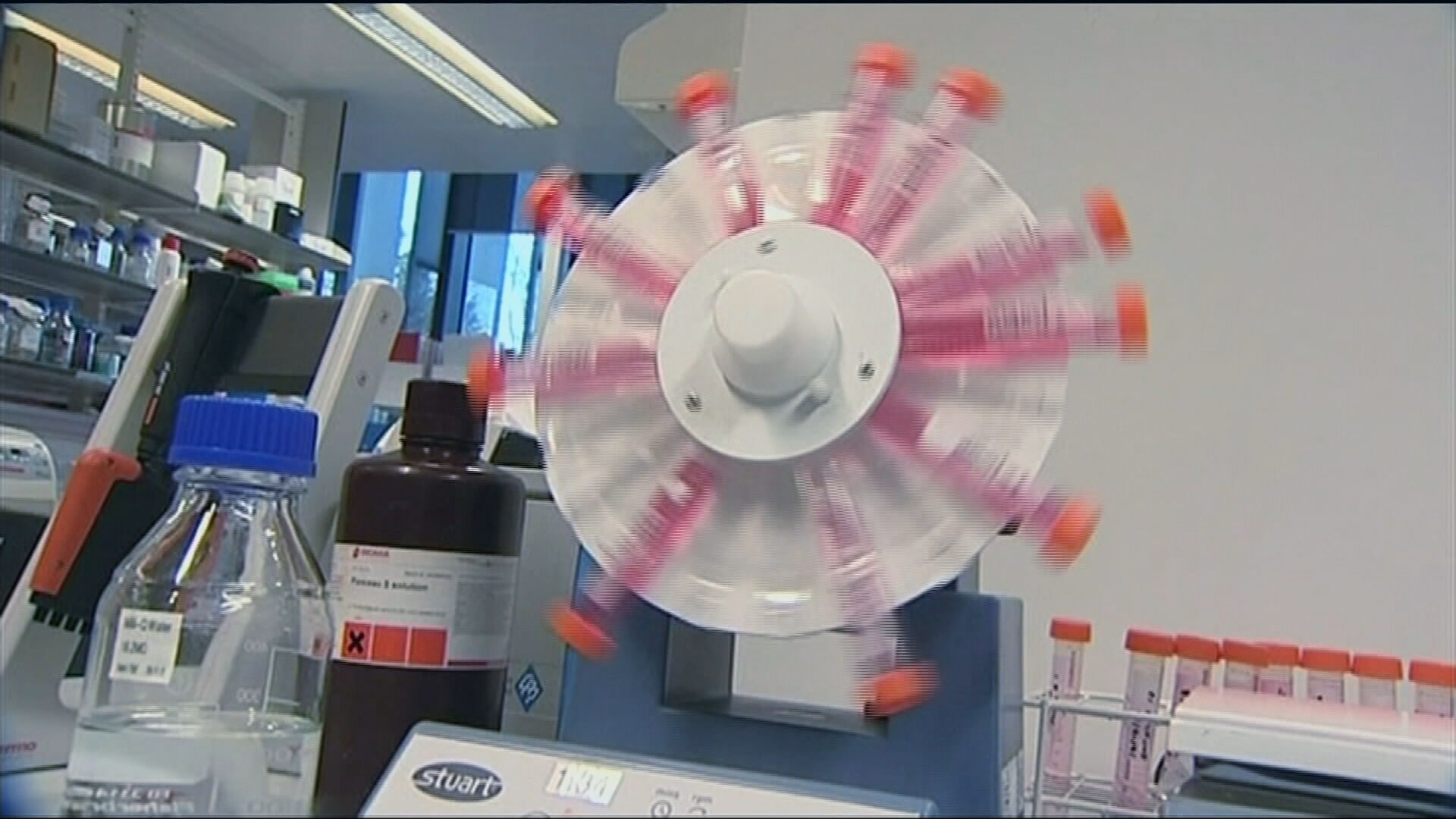
Approved on the NHS, the ROCA test has now been rolled out at University College London Hospitals NHS Foundation Trust (UCLH) in London, with plans to extend it across England.
The test assesses changes in a woman’s serum CA125, which could indicate the cancer was present.
Heightened risk
Women with the BRCA genes 1 and 2 are at a heightened risk of breast and ovarian cancer. With breast cancer, women can have mammograms to screen for the disease. There is nothing similar for ovarian cancer.
Professor Adam Rosenthal, consultant gynaecologist at UCLH, said the new test was designed as a damage limitation option for women who are not yet ready to have surgery.
A raised test means they can then re-assess whether they are ready to have their ovaries removed.
For these women, it has the added advantage of catching the cancer early, giving them a greater chance of survival.


Natasha’s story
Natasha Wray was found to have the BRCA gene after being treated for breast cancer and she was advised to have her ovaries removed.
“I was 36 at the time, and I said, absolutely not. I’d just gone through seven rounds of chemo, extensive surgery, and had sort of a year and a half, two years of my life caught up in cancer treatment, and I just wanted to be left alone,” she said.
“And I also didn’t want to go through a surgical menopause in my mid-30s. I also very much wanted to be a mum, so I definitely wanted to hold on to any fertility that I did have.”
“I didn’t want to go through a surgical menopause in my mid-30s. I also very much wanted to be a mum.”
– Natasha Wray
Having the tests, which she had to initially pay privately for, did come with anxiety but Professor Rosenthal said it means the question of when to have the surgery was at the forefront of their minds.
At 41, Natasha had a baby and two years later had some results which showed raised levels of CA-125. Even then she waited a while longer.
“It wasn’t easy, “she said. “But I do think it’s really important as well that women’s bodies aren’t just seen as baby making bodies and machines. I very much wanted to be a mother. That wasn’t my sole purpose for holding onto my ovaries.


“It was very personal and it actually had nothing to do with anybody else. It was very much me, how I felt in my body, what had already been felt like to me, taken from me.”
The ROCA test has been approved by the National Institute for Health and Care Excellence (NICE) for carriers of the BRCA genes and with the results also showing it is cost-effective, it is hoped it will be made available across England.
Watch more here:
Experts sceptical as Trump to link paracetamol in pregnancy to autism
Doctors found guilty of sexual misconduct allowed to keep practicing
Maternity failures: 14 NHS trusts to be investigated in national inquiry



